For the past year, governments and policymakers around the world have attempted to deal with the Coronavirus Disease 2019 (COVID-19) pandemic through a variety of methods. These include implementing controversial lockdowns and stay-at-home orders. The degree to which these measures have helped to slow the spread of COVID-19 is still debated, but experts agree that the mental, physical, and financial wellbeing of individuals has been impacted.
There has been an alarming rise in the rates of domestic violence, suicide, drug overdose, and substance abuse over the past year, with strong ties to lockdowns, unemployment, and stress.
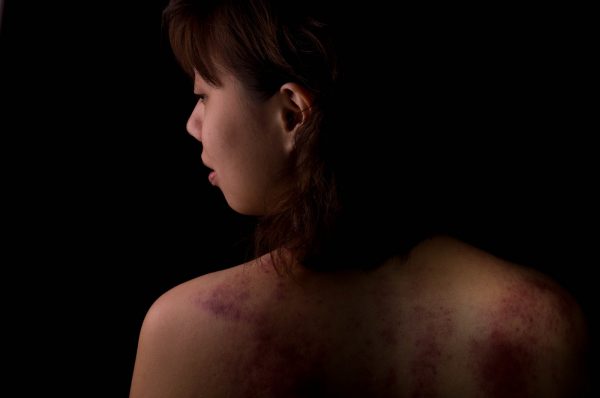
COVID-19 lockdown consequences: domestic violence
“Domestic violence incidents in the U.S. increased by 8.1% following the imposition of stay-at-home orders,” according to a systematic review and meta-analysis conducted by the nonpartisan National Commission on COVID-19 and Criminal Justice (CCJ). Worldwide, an average 7.9 percent increase in reported domestic violence was observed. The pooled studies analyzed a wide array of data sources, including police logs, emergency hotline registries, health records, and other administrative documents.
While the authors were unable to pinpoint the exact drivers of the 2020 spike in domestic violence, they stated that “lockdowns and pandemic-related economic impacts may have exacerbated factors typically associated with domestic violence, such as increased unemployment, stress associated with childcare and homeschooling, and increased financial insecurity.” Reporting signs of abuse and offering help to victims also became more difficult because parents and children were isolated in homes, away from friends, neighbors, and teachers who could sound an alarm.
In response to the spike in domestic violence against children, 21 leaders of organizations around the world, such as the World Health Organization (WHO) and United Nations International Children’s Emergency Fund (UNICEF), submitted a joint statement in April 2020 calling for action. The CCJ highlighted the need for additional resources for abuse prevention and victim services, especially for historically marginalized groups such as “older adults, women, and children with past experiences with violence and abuse, as well as those with ongoing mental illness and chronic health conditions.”
Suicide and mental health disorders
Success
You are now signed up for our newsletter
Success
Check your email to complete sign up
Mental health challenges have been devastating during the COVID-19 pandemic, according to results from a June 2020 Centers for Disease Control and Prevention (CDC) study. “Overall, 40.9% of respondents reported at least one adverse mental or behavioral health condition, including symptoms of anxiety disorder or depressive disorder (30.9%), symptoms of a trauma- and stressor-related disorder (TSRD) related to the pandemic† (26.3%), and having started or increased substance use to cope with stress or emotions related to COVID-19 (13.3%).”
While 10.7 percent of all respondents aged 18 and older had “seriously considered suicide” within the past 30 days, the percentage was significantly higher at 25.5 percent for respondents aged 18 to 24 years. In 2018, only 4.3 percent of surveyed adults had thoughts of suicide.
Unprecedented numbers of suicides during the pandemic have shocked physicians such as Dr. Mike deBoisblanc, head of the trauma department at John Muir Medical Center in California. In May 2020, he stated, “I think, originally, this (the shelter-in-place order) was put in place to flatten the curve and to make sure hospitals have the resources to take care of COVID patients.” However, he said, “We’ve never seen numbers like this, in such a short period of time. I mean we’ve seen a year’s worth of suicide attempts in the last four weeks.”
Critics of lockdowns have cited a 2011 study that examined the relationship between employment status and suicide risk in the U.S. from 1996 to 2005. Unemployment duration was found to be the “dominant force in the relationship between job loss and suicide,” and the authors found that “mass-layoffs may be powerful localized events where suicide risk increases shortly afterward.” Moreover, a 2003 cohort study in New Zealand concluded that unemployment was associated with a “twofold to threefold increased relative risk of death by suicide, compared with being employed.”
A 2020 analysis titled “Projected Deaths of Despair from COVID-19” was conducted by Well Being Trust (WBT) and the Robert Graham Center for Policy Studies in Family Medicine and Primary Care. Based on 2018 baseline data, projected unemployment rates from 2020 to 2029, and nine different scenarios, the number of projected additional annual “deaths of despair” due to the COVID-19 recession range from 27,644 to 154,037.
“Deaths of despair” include deaths from suicide, drug abuse, and alcohol abuse. Major factors for the increase include “unemployment, mandated social isolation for months and possible residual isolation for years.” In addition, the authors emphasize that isolation, “whether called social isolation or physical distancing is leading to loss of social connection and cohesion.”
School closures have also negatively affected households. Dr. Robert Redfield, former CDC director, said during a medical webinar in July 2020 that “there has been another cost that we’ve seen, particularly in high schools. We’re seeing, sadly, far greater suicides now than we are deaths from COVID.” He described the consequences of prolonged school closures and stressed that health must encompass the “overall social being of individuals.”

Drug overdoses and substance abuse
Substance abuse, a well-known coping mechanism for stress, increased significantly during lockdowns. A recent study published in Feb. 2021 in Psychiatry Research found that over the six month period from April to Sep. 2020, “hazardous alcohol use and likely dependence increased month-by-month for those under lockdowns compared to those not under restrictions.” Percentages of individuals under lockdown that met the cutoffs for “harmful alcohol use” increased from 21.0 percent in April to 40.7 percent in September, but the corresponding percentages for individuals not under restrictions “were essentially unchanged.”
Factors that were associated with greater alcohol consumption included “younger age, male sex, and primary job loss due to COVID-19,” with job loss exerting the greatest influence. Lockdowns and stay-at-home restrictions were associated with drastic increases in high-risk drinking, likely associated with a broad range of stressors, such as managing children at home, financial hardships, social isolation, and disrupted routines.
Furthermore, staying at or working from home offers easier access to alcohol, which could lead to less motivation, poor judgment, and increased errors. Alcohol misuse has “long-term health implications,” which include “elevated rates of injuries, liver disease, cancer, somatic problems, psychiatric conditions, and all-cause mortality.”
According to a preliminary report by the nonpartisan American Institute of Economic Research (AIER) regarding the cost of lockdowns based on data from research journals, the CDC, and other organizations, the “US had over 81,000 drug overdose deaths in the 12 months ending in May 2020, the highest number ever recorded in a 12-month period.” In late June 2020, a CDC study showed that 13.3 percent of U.S. adults “started or increased substance use to cope with stress or emotions related to COVID-19.”
The American Medical Association (AMA) reported in an article updated on March 3, 2021, that over 40 states had reported “increases in opioid-related mortality.” While all these profound negative impacts on mental health and the ability to combat addictive and abusive behaviors can be attributed to social isolation and lockdowns, the benefits of such measures remain a question.
Follow us on Twitter or subscribe to our email list
















