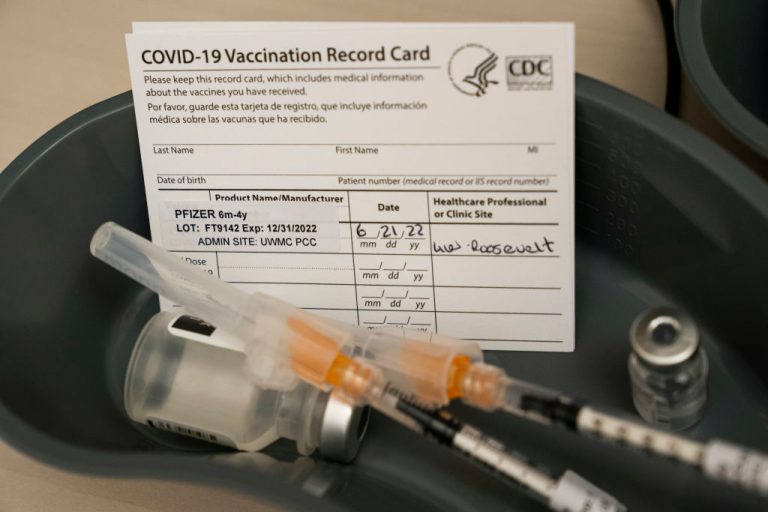
How long does protection from COVID-19 vaccines last, and how often are boosters needed? Does getting an infection or getting a vaccine afford better protection against reinfection and severe disease?
Constantly evolving conditions and new variants have made these questions difficult to answer. Centers for Disease Control and Prevention (CDC) data showed that the BA.4 and BA.5 Omicron variants accounted for nearly 95 percent of new U.S. Coronavirus Disease 2019 (COVID-19) cases in the week ending on July 23, compared to early May when the two variants made up less than five percent of cases.
FDA statement
The U.S. Food and Drug Administration (FDA) issued a statement on June 30 citing concerns about the efficacy of current vaccines against “circulating and emerging variants.” During an in-depth discussion on June 28, an “overwhelming majority” of advisory committee attendees favored altering COVID-19 vaccines to be used for boosters in the U.S. in the fall.
The agency stated, “We have advised manufacturers seeking to update their COVID-19 vaccines that they should develop modified vaccines that add an omicron BA.4/5 spike protein component to the current vaccine composition to create a two component (bivalent) booster vaccine, so that the modified vaccines can potentially be used starting in early to mid-fall 2022.”
The FDA continued, “Vaccine manufacturers have already reported data from clinical trials with modified vaccines containing an omicron BA.1 component and we have advised them that they should submit these data to the FDA for our evaluation prior to any potential authorization of a modified vaccine containing an omicron BA.4/5 component.”
Success
You are now signed up for our newsletter
Success
Check your email to complete sign up
The agency said it had requested manufacturers to initiate clinical trials on the dual-spike product.
Shares of Moderna increased by 3.8 percent after the company announced on July 26 that the U.S. government would pay up to $1.74 billion to deliver 66 million doses of boosters offering better protection against the BA.4 and BA.5 Omicron subvariants.
Pfizer and BioNTech had already signed a deal with the U.S. government in June for $3.2 billion for 105 million doses of an Omicron-adapted vaccine.
Waning immunity
How long does protection from COVID-19 vaccines last? According to a Qatar study published in the journal Nature on June 2, mRNA COVID-19 vaccines have waning efficacy months after each jab.
The study spanned Dec. 23, 2021 to Feb. 28, 2022, when infections were dominated by the BA.1 and BA.2 Omicron subvariants.
While the second dose of the Pfizer-BioNTech vaccine was 47.8 percent effective against any symptomatic Omicron infection during the first 1 to 3 months, the efficacy declined to 16.3 percent after 4 to 6 months and then to -9.0 percent after 7 months.
In other words, 7 months after the second dose of the vaccine, people were more likely to have symptomatic COVID-19 compared to unvaccinated individuals.
Protection was enhanced by the third dose of the Pfizer-BioNTech vaccine, with up to 55.5 percent efficacy 2 to 3 weeks after the jab, but booster efficacy declined to 21.9 percent by 14 weeks.
Even when separating the results by BA.1 and BA.2 Omicron subvariants, the results did not change significantly.
The Moderna COVID-19 vaccine also showed a similar decline in efficacy, from 43.2 percent 1 to 3 months after the second dose to 18.7 percent 4 to 6 months after the jab and -13.7 percent by 7 months.
Like the Pfizer vaccine, at 7 months after the second dose, people were more likely to have symptomatic COVID-19 compared to unvaccinated individuals. Dose 3 of the Moderna vaccine was 53.7 percent effective 2 to 3 weeks after the injection, but declined to 34.9 percent after just 6 weeks.
Natural immunity, severe disease, and reinfection
What about the effectiveness of the vaccines against reinfection or severe Omicron infection compared to natural immunity? The Qatar study authors found effectiveness against “severe, critical, or fatal COVID-19 due to an Omicron infection” to be “in the range of 70–80% at any time after the second dose for both the BNT162b2 and mRNA-1273 vaccines.”
They added, “However, BNT162b2 effectiveness against any severe, critical, or fatal COVID-19 after the booster dose was greater than 90%.”
Immunity granted by natural infection against reinfection and severe disease was explored in a preprint article by the same Qatar team.
The paper has not yet been peer-reviewed, but was published July 7 on medRxiv. The researchers found effectiveness “of pre-Omicron primary infection against pre-Omicron reinfection was 85.5%,” peaking at 90.5 percent “in the 7th month after the primary infection, but waned to ∼70% by the 16th month.”
The Omicron variant appeared to be more easily spread, as effectiveness “of pre-Omicron primary infection against Omicron reinfection was 38.1%… and declined with time since primary infection.”
However, natural immunity offered superior protection “against severe, critical, or fatal COVID-19 reinfection,” with an effectiveness of 97.3 percent “irrespective of the variant of primary infection or reinfection, and with no evidence for waning.”