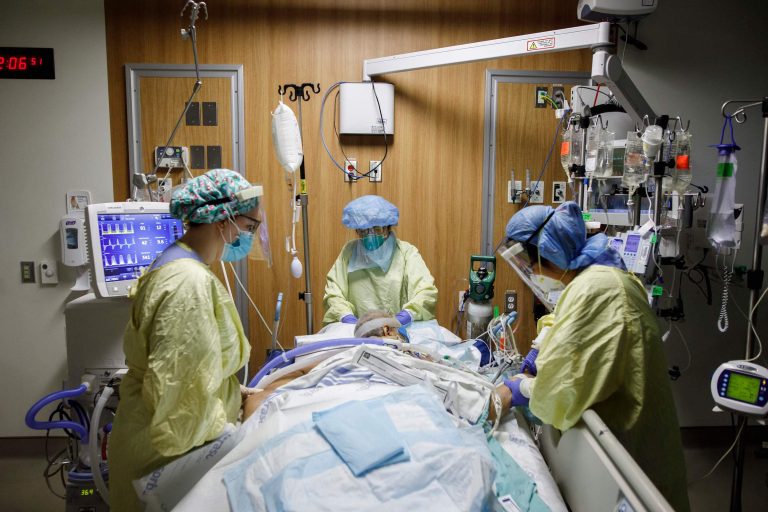
The wait times for patients to see a specialist, obtain diagnostic procedures, or undergo surgery in Canada now reach the highest in nearly three decades, according to a new report by the Fraser Institute.
“Waiting for treatment has become a defining characteristic of Canadian health care,” the Fraser Institute said in its news release on Dec. 8. Entitled “Waiting Your Turn: Wait Times for Health Care in Canada, 2022,” the report was based on the think tank’s effort in the nearly 30 years to document how long it takes for Canadian patients to receive necessary medical treatment.
The researchers collected data from Jan. 10 to Sept. 15 — a longer period of time than preceding years—and surveyed specialist physicians across 10 provinces, from 12 specialties, to find the median waiting time between referral from a general practitioner and receipt of treatment.
According to the report, this year, an estimated 1,228,047 Canadians are waiting for procedures in 10 provinces. This means, if each person waits for only one procedure, then roughly 3.2% of Canadians are waiting for treatment in 2022.
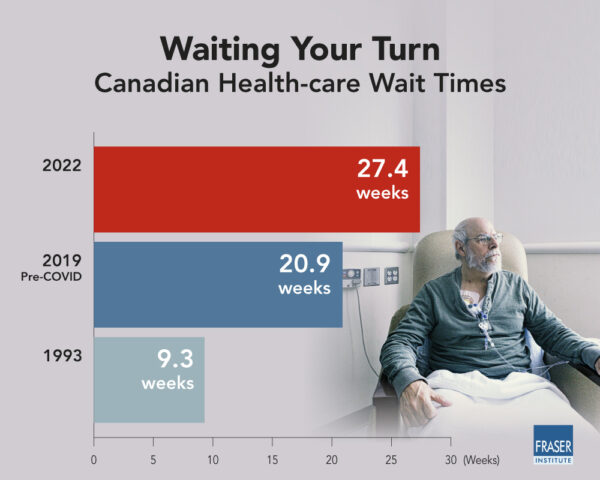
The wait time this year reaches record high, which is 27.4 weeks, or 195 percent longer than the median waiting time of 9.3 weeks in 1993, longer than the wait of 25.6 weeks in 2021, and longer than the wait of 20.9 weeks in 2019, the year before COVID.
Success
You are now signed up for our newsletter
Success
Check your email to complete sign up
Across the country, wait times vary substantially by province. Ontario reports the shortest total wait—20.3 weeks—while Nova Scotia reports the wait 58.2 weeks, second to Prince Edward Island, which reports 64.7 weeks, the longest.
The total wait time that patients face typically include two segments, one is from referral by a general practitioner or family doctor to consultation with a specialist and the other is from the consultation with a specialist to the point at which the patient receives treatment.
The wait time to see a specialist after receiving a referral has increased from 11.1 weeks in 2021 to 12.6 weeks in 2022 which is 242% longer than in 1993, when it was 3.7 weeks. The shortest waits for specialist consultations are in Ontario (10.1 weeks) while the longest occur in Prince Edward Island (41.7 weeks).
The waiting time following consultation with specialist increased from 14.5 weeks in 2021 to 14.8 weeks this year which is 164% longer than in 1993 when it was 5.6 weeks, and 6.7 weeks longer than what physicians consider to be clinically “reasonable” (8.1 weeks). Ontarians have the shortest specialist-to-treatment waits (10.2 weeks), while Manitobans have the longest (25.4 weeks).
The length of the wait is dependent on specialty or the type of procedure patients need to go through.
Patients undergoing radiation treatments wait 3.9 weeks, while those who need a neurosurgical procedure wait the longest, more than a year, at 58.9 weeks.
For those who need elective cardiovascular surgery, the wait time is 16.4 weeks, while plastic surgery patients wait 58.1 weeks, and orthopedic surgery patients wait 48.4 weeks.
Patients also experience significant waiting times for various diagnostic technologies.
Those who need a computed tomography (CT scan) can expect to wait 5.4 weeks this year. The wait for magnetic resonance imaging (MRI) is almost double, at 10.6 weeks, while the wait for an ultrasound is 4.9 weeks.
New Brunswick had the longest waits for CT scan (8.0 weeks), Prince Edward Island had the longest waits for both MRI (20.0 weeks) and an ultrasound (24.0 weeks).
“Wait times can, and do, have serious consequences such as increased pain, suffering, and mental anguish. In certain instances, they can also result in poorer medical outcomes— transforming potentially reversible illnesses or injuries into chronic, irreversible conditions, or even permanent disabilities,” write authors Mackenzie Moir and Bacchus Barua.
“In many instances, patients may also have to forgo their wages while they wait for treatment, resulting in an economic cost to the individuals themselves and the economy in general.”
Dying while waiting
Following the Fraser Institute report showing record high wait times, SecondStreet.org released its new Died on a Waiting List report on Dec. 13 after gathering and analyzing government data on patients dying while waiting for surgery and diagnostic scans.
According to SecondStreet.org, there has been a 24% increase in surgical waiting list deaths, a four-year high since the organization began tracking this problem in 2018-19. Information obtained from Ontario Health data shows an increase of over 400% when it comes to waiting list deaths for CT scans and MRI scans since 2015-16.
At least 13,581 patients died while waiting for surgeries, procedures, and diagnostic scans in 2021–22, SecondStreet.org said. That’s up from 11,581 last year. More than 10,000 of the deaths this past year were people waiting for diagnostic scans.
The report said the deaths fall into two categories: one is people who died because they did not receive the needed treatment or diagnosis; the other is people who died of other conditions while awaiting diagnosis or treatment for non-life-threatening conditions. Although the latter group did not die because of the delay, their quality of life in their final days may have been impacted, said the report.
Earlier in November, the Canadian Association of Radiologists (CAR) published a report titled “Improving Access to Lifesaving Imaging Care for Canadians.” It said: “Before the pandemic, Canadians were waiting an average of 50 to 82 days for CT scans and up to 89 days for MRI imaging. This is 20 to 52 days longer than the recommended 30-day wait time for these potentially lifesaving modalities. During COVID, waitlists lengthened, creating ominous circumstances for people needing cancer screening, or patients requiring image-guided therapies or ongoing management of their disease.”