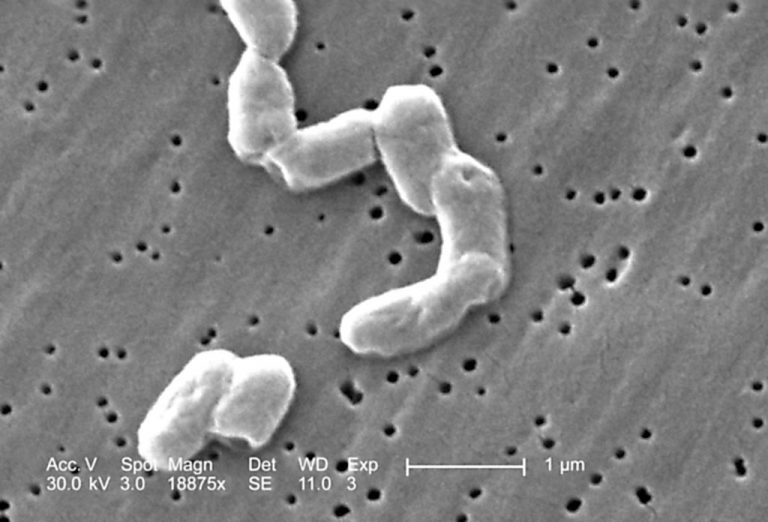
The CDC has potentially identified the source of a salmonella outbreak, which is still of “unknown origin” as the CDC continues to track the spread of the bacteria. While still not officially confirmed, the bacteria was discovered in a “takeout condiment cup”, which included cilantro, limes, and onions. According to local Florida news media, the sample alluded to may be limited to only one takeout cup from one person who fell ill. The ill person indicated that no onions were left in the cup at the time that they brought the sample for analysis.
A brief review of the most recent salmonella outbreaks as well as those that generated heavier media coverage over the past 15 years was compared with the present heavily-covered case to explore potential vectors for this most recent outbreak. While the source of the current suspected contaminant “takeout cups” has not been revealed by the CDC, it was noted by the CDC that the condiment cups contained cilantro, lime, and onion. In 2016, the popular chain Chipotle temporarily closed 2,000 stores to control an outbreak of salmonella, E. coli, and norovirus. This was one source among those reviewed; the others are listed below, further in the text. The popular burrito chain Chipotle is noted for its takeout, which includes fresh condiments, including the three listed by the CDC. However, this does not yet fully indicate that Chipotle is determined to be the source of the outbreak. A reddit thread on the topic includes comments indicating that the chain has garnered some suspicion among a few netizens regarding being a potential source of the outbreak. This includes some who may be employees; while these comments are not definitive, they do suggest that connecting the fresh food chain to the condiment cups may not be a stretch. Says one netizen, sarcastically, “I love how they think it’s a big mystery”.
A Widespread Outbreak
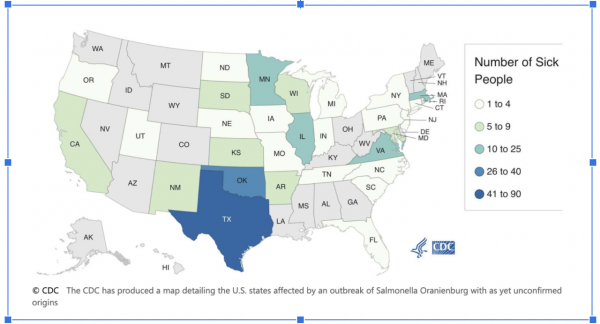
The multi-state outbreak of Salmonella Oranienburg infections is concentrated mainly in Texas, where 81 people were sickened, and Oklahoma, with 40 victims. However, infections have been reported in at least 29 additional states, including those as far away as Massachusetts, Wisconsin, and Virginia, where 22 people were sickened. The CDC warns that many people recover without treatment and are not tested for salmonella, so the outbreak is likely more widespread than has been confirmed. The bacteria has sickened 279 confirmed people since September 23; of these, 26 required hospitalization.
According to the CDC, Salmonella bacteria cause approximately 1.35 million infections, 26,500 hospitalizations, and 420 deaths per year in the United States alone. The FDA estimates that over 90 million infections occur worldwide each year. The infection vector is usually foodborne,
Recognizing the onset of salmonella poisoning
Symptoms of salmonella poisoning include stomach cramps, fever, and diarrhea, and usually begin 6 hours to 6 days after infection and last 4 to 7 days. Many people recover without special treatment. Dehydration, fever-related complications, and weakness from lack of nourishment are some of the more dangerous outcomes related to the sickness. Young children, the elderly, pregnant women, and those with pre-existing conditions should be monitored carefully; please consult healthcare providers if needed. The CDC does not recommend antibiotics, except in extreme cases.
Success
You are now signed up for our newsletter
Success
Check your email to complete sign up
The Mayo Clinic reports that most people contract salmonella poisoning, called salmonellosis, by eating foods that are contaminated with fecal matter, as salmonella bacteria live in the intestines of animals and people. The bacteria can also be transmitted by insects, such as the common housefly. The FDA says that salmonellosis is the second leading cause of foodborne illness, following norovirus.
Preventing contamination
Preventing salmonella contamination in the kitchen centers around surface cleaning, as well as not re-using food handling surfaces and tools such as cutting boards and knives before they are sanitized, and the adequate cooking of raw foods. If salmonella contamination is suspected, it is recommended to use a cleaner of appropriate strength, such as a diluted bleach solution. Bar mops and reusable kitchen cloths as well as table linens can also be soaked in an appropriate solution. More tips can be found here, provided by a consumer food safety non-profit, the Partnership for Food Safety Education.
Leafy greens and other fruits and vegetables consumed raw present a danger, as they can transmit salmonella more readily than food that has been thoroughly cooked.
Kitchen culture changed greatly after an increased awareness of salmonella bacteria that can be carried in and on raw eggs. For instance, children in the 1950s would lick beaters or the bowl leftover from cookie or cake batter; this is no longer the case. Additionally, it is now recommended to cook the meat right out of the package without rinsing it first, as the FDA suggests that the risk of foodborne diseases from the process of washing — perhaps, from water spattered while cleansing raw meat — is actually greater than the contamination risk if the meat is properly cooked immediately out of the package.

But what are the “usual suspects” of salmonella outbreaks?
Greens have been the culprit in past outbreaks in recent history. But so has milk packaged for infants, in Europe, leading to an international recall in 2018. In 2010, egg prices on the west coast of the United States rose more than 40 percent after two Iowa egg farms recalled more than half a billion eggs suspected of contamination with salmonella. The number of people believed sickened by the eggs was 1,300. And in 2009, the FDA issued a warning after a central California pistachio processor voluntarily recalled the nuts due to worries over potential contamination. In February of 2016, the popular chain Chipotle closed its nearly 2,000 restaurants across the US for several hours as a team assessed how to handle an outbreak in its restaurants of salmonella, E. coli, and norovirus.
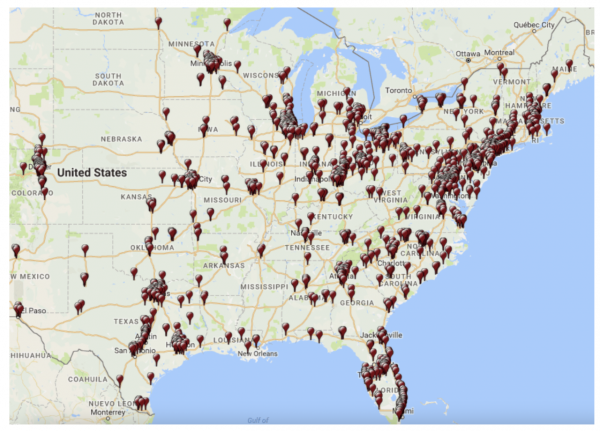
Staying safe with food delivery services
The CDC is currently turning its investigation to “takeout cups” containing fresh condiments including cilantro, onions, and limes, but the Partnership for Food Safety Education has been recently warning consumers about takeout and delivery in general, due to its increased popularity in these present times.
The ongoing pandemic as well as other factors have placed food delivery “on the rise,” says the Partnership for Food Safety Education. Delivered items include meal kits, restaurant delivery, and grocery delivery. This has also increased the public’s chances of exposure to contaminated food due to the timing involved in the delivery process.
The Partnership recommends making sure that someone is at home to receive food when it is delivered to prevent it’s sitting out of the refrigerator or safe storage. If a recipient meeting the delivery cannot be arranged, it’s recommended to take time to ensure a shady place free of pets or rodents in order to protect your delivery until you arrive. The “danger zone”, at which microorganisms multiply rapidly in food is between 40 and 140 degrees Fahrenheit. Items containing fresh dairy and items containing fresh tomatoes are especially susceptible to spoilage and contamination.
Finally, examine delivered food for stickers or notices indicating that it is perishable or that it must be kept refrigerated or frozen, and check to be sure meats and dairy items do not show signs of leaking, which could indicate compromised packaging and possible contamination.
Other sources of infection
Infection can also come from poor hand washing and a variety of other factors, usually related to hygiene and often associated with animal contact. In fact, the name itself hails from the name of Dr. Daniel E. Salmon, a veterinarian who made a career of studying animal diseases for the US Department of Agriculture. Salmonella infections can occur from handling animals, including dogs, cats, and rodents fed to reptiles, and can also be carried on the outside of cages and aquariums.